Bunions
What is a bunion (Hallux Valgus)?
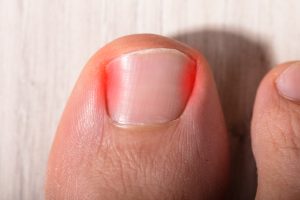
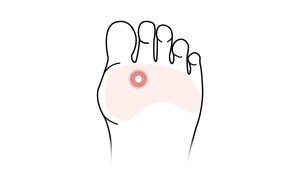
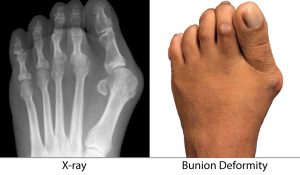
Bunions to the big toe, or the medically termed Hallux Valgus, is a progressive deformity of the big toe resulting in widening of the forefoot and gradual dislocation of the big toe towards the second. The overlying skin maybe swollen, red and tender. Bunions are often painful and can limit what shoes you can wear
Causes of bunions:
Bunions are a common occurrence in men and women and typically start progressing in their teens. It is well agreed amongst foot specialists that a strong genetic link exists in most cases.
More than 50% of Women in the UK have bunions, therefore it is a common foot deformity. The problem often runs in families, although tight narrow shoes and high heels are often blamed.
Symptoms of bunions:
- A bulge or bump on the outside of your big toe
- Pain and swelling around the big toe joint
- There may be hardened skin or a callus on the bump
Diagnosing bunions:
Our hallux valgus/ bunion specialist, Mr Kaser Nazir, will refer for X-rays at the time of your initial consultation to determine the size and angle of your bunion deformity. This will allow him to offer the most suitable bunion treatment to correct and align the bunion.
Hallux Valgus Surgery:
- Scarf and akin osteotomy – the procedure can be carried out under local anaesthesia or sedation as a day case. The bunion bump is shaved down, the metatarsal cut and joint realigned. Following this screw fixations are used to keep the bone in position. A small wedge of the phalanx is removed, closed and fixed to allow the toe to heal in the aligned position. Over the first two weeks you should rest at home, during this period you can partially mobilise with the aid of crutches. Typically you can return to high impact activities between 6-8 weeks following surgery.
- Minimally invasive bunion correction – The minimally invasive bunion correction or keyhole bunion surgery is similar to the scarf and akin osteotomy. Using an imaging intensifier (X-rays) our experienced surgeon can carry out the procedure with tiny incisions. Specialised screw fixations are used during the procedure to keep the aligned toe in position whilst it heals. We advise on two weeks rest at home whilst you partially mobilise with the aid of crutches. Typically high impact activities can start between 6-8 weeks following surgery.
- Lapidus procedure – For more severe bunions our specialist may advise on the lapidus arthrodesis procedure. An incision is made at the top of side of your foot where the bony growth is removed. The joint near the instep (tarsometatarsal joint) is realigned and fused with fixations, typically a plate, screws and/or an implant. Over the first 2 weeks following surgery you should rest at home with your leg elevated to promote healing. After two weeks you will be transitioned in to an aircast boot for a further 4-6 weeks. Typically you will be able to return to high impact activities at 3 months following surgery.
Find out information on Tailor’s bunion deformity
Frequently asked questions
The causes of a bunion is multifactorial, mainly people are genetically predisposed to them. Factors such as tight pointy foot wear can speed up the process of the condition.
The only way to reverse a bunion is with surgery that can be carried out as a day case procedure. Common procedures include the scarf and akin osteotomy or the minimally invasive bunion correction. For more severe bunions, a lapidus procedure may be suggested. Your surgeon will refer for X-rays to determine the most appropriate option for you.
The bunion cannot be corrected without surgery but some splints can hold the toe to improve the alignment if this helps with symptoms. Additionally, orthotics can be made for your shoes to help with your foot function.
The fastest way to get rid of a bunion is with surgery. The modern procedures have very good outcomes and they can be done minimally invasively.
Related Blogs
Thoughts and advice on foot health care from the Podogo team.